Current Options for Managing Canine Osteoarthritis
A host of effective modalities are available for alleviating discomfort and improving mobility in dogs with degenerative joint disease.
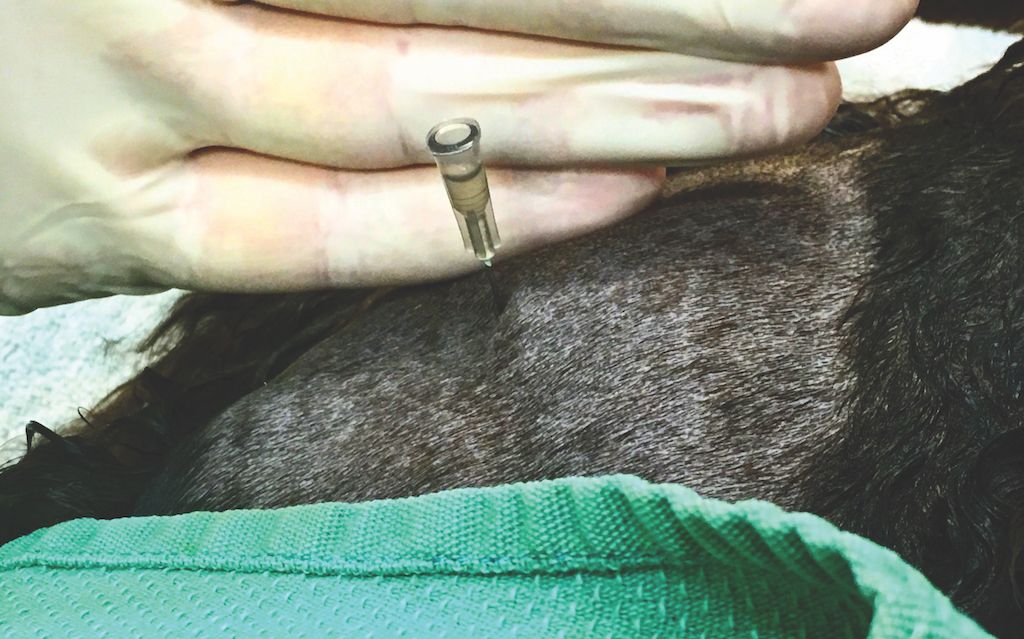
Intra-articular needle placement for the hip joint. The joint fluid in the hub of the needle indicates correct placement.
David Dycus, DVM, MS, CCRP, DACVS-SA, is on a mission. He wants to help his fellow veterinarians understand that managing canine osteoarthritis (OA) is not a matter of simply prescribing a pain reliever and an anti-inflammatory and sending patients on their way. Instead, he said, managing this chronic, painful condition requires a patient-specific, multipronged approach.
RELATED:
- The Gold Standard for Managing Canine Osteoarthritis
- PRODUCT NEWS: New Drug Available for Canine Osteoarthritis
“At the end of the day, it’s all about keeping patients comfortable so they can stay active, maximize range of motion, and maintain lean body weight,” said Dr. Dycus, an orthopedic staff surgeon at Veterinary Orthopedic & Sports Medicine Group in Annapolis Junction, Maryland, and cofounder/codirector of the Veterinary Sports Medicine and Rehabilitation Institute. “If our patients aren’t comfortable, they’re not going to be active.” And with inactivity, he said, comes weight gain, stiffness, and loss of range of motion.
But this vicious circle can be broken with the help of several existing and new treatment modalities. American Veterinarian® spoke with Dr. Dycus about today’s best practices for managing OA.
What is your overall approach to the patient with OA?
David Dycus, DVM, MS, CCRP, DACVS-SA: In people with OA, most of the stiffness, soreness, and pain come from the loss of range of motion, and I think the same probably applies to dogs. If we can maintain as much range of motion as possible and exercise them daily, they’re going to have less stiffness and more comfort.
It used to be that we prescribed an anti-inflammatory and there wasn’t much more we would do. What has emerged in the past decade or so is the concept of multimodal management, the idea that anti-inflammatories can be combined with other modalities to better manage the condition.
We have to come at OA from every angle, with the ultimate goal of maintaining comfort and daily exercise for the dog. Owners don’t want to think they are hurting their pets, so it’s our job to ensure they stay comfortable and exercise to maintain range of motion and ideally minimize or slow disease progression as best as possible. And exercise doesn’t mean going into the backyard and chasing squirrels. It means getting outside and going on walks. Ideally, most dogs should be able to go comfortably on at least two 20-minute leash walks on flat ground every day. Once they can achieve this, then the sky is the limit in terms of time, distance, terrain, and elevation.
To achieve that level of comfort, we combine various modalities, typically starting with pain management.
Evaluating and Managing Pain
How do you manage their pain?
Just as in people, dogs with OA have periods of relative calmness and then periods of flare-ups during which clinical signs are acutely exacerbated. It is during the periods of calmness where we have our “baseline [management] approach.” This includes joint supplements such as glucosamine, chondroitin, and omega-3 fatty acids. However, the most important aspect of the baseline approach is daily exercise and maintenance of a lean body weight. If a patient with OA deviates from its baseline, this can indicate a flare-up. When this happens, we take a step back and ask ourselves what we can do to get the flare-up under control so that the patient can return to its baseline. During a flare-up there is more pain and discomfort, so step 1 is getting this under control.
We may start with pharmaceuticals such as nonsteroidal anti-inflammatory drugs (NSAIDs), but the goal is to use these at the lowest dose and as infrequently possible. This means using an NSAID for 10 to 14 days during the early phases of OA knowing that at some point in the future the patient may need daily NSAID support. As a profession, we’ve got to move away from offering only an anti-inflammatory and an opioid and thinking there is nothing more we can do.
Other pharmaceuticals that can be considered are opioids such as codeine. However, it should be remembered that opioids are not designed for chronic use. Gabapentin, amantadine, and amitriptyline, among others, can be considered along with an NSAID.
Do you prescribe tramadol for pain management?
I’ve moved away from tramadol for joint pain. I think there has always been controversy over tramadol’s effectiveness, with no real clinical evidence that it was helpful, and there seems to be a consensus now that it doesn’t work very well to control joint pain. One recent study used both positive and negative controls (placebo) and found that there was no improvement in peak vertical force or vertical impulse in dogs on tramadol versus placebo.1 Rather than it being a true opioid and controlling pain, I think tramadol likely affects serotonin levels. So the patient may be a bit spaced-out, but they are probably still painful.
Is grapiprant effective?
Grapiprant (Galliprant; Elanco) is a prostaglandin-receptor antagonist that targets the EP4 receptor that’s involved in OA-associated pain and inflammation. Formulated only for dogs, grapiprant can help animals that haven’t tolerated or responded to traditional NSAIDs. It’s also associated with fewer hepatic, renal, and gastrointestinal side effects. It might be a good go-to for some of those older patients who are stuck between a rock and a hard spot because they can’t tolerate traditional anti-inflammatories.
In what other ways can pain be kept under control?
There are a lot of avenues beyond pharmaceuticals to make these patients comfortable. Other disease-modifying OA agents, such as joint supplements with glucosamine, chondroitin, omega-3 fatty acids, and polysulfated glycosaminoglycans, can be incorporated, for example.
Adding to our multimodal management approach during a flare-up is the incorporation of formal physical rehabilitation and intra-articular injections. Physical rehabilitation can be used to allow active muscle contractions while minimizing the stress being placed on the joints. In this situation we can allow a patient to remain active and thus maintain range of motion while simultaneously working to help get pain under control. Rehabilitation therapies are a great nonpharmaceutical avenue for managing pain and in many cases can help us lower the dose or frequency of pharmaceuticals.
Intra-articular injections include a variety of substances, such as steroids, hyaluronic acid, or regenerative medicine (platelet-rich plasma [PRP] and/ or mesenchymal stem cells). Intra-articular injections are a way to further reduce the inflammatory response in a more target-directed way over the oral analgesics. These products can achieve a high concentration directly at the joint.
Once they’re comfortable we get them back to their baseline. It’s important to remember that what works during one flare-up may not work for the next. We must always be evolving and taking a multimodal, patient-centered approach rather than a cookbook approach.

Therapeutic ultrasound can be used prior to beginning a rehabilitation session to warm up tissues for easier stretching.
Rehabilitation Therapy
How do you incorporate rehabilitation into the treatment plan?
Manual therapies like stretching and range-of-motion exercises can help during the initial phases of rehabilitation when patients are still painful. In addition, we can add in cryotherapy and warm packing during various situations to further help with our manual therapies.
In addition to manual therapies, therapeutic exercises can be used initially to help with balance and proprioception. These exercises can include wobble boards, peanut balls, and balance balls. Once the patient is comfortable we can use therapeutic exercises to increase muscle strength and improve endurance. This can be accomplished with things such as cavalletti poles, sit-to-stand exercises, dancing exercises, and many others.
Therapeutic modalities such as electrical stimulation, shockwave, and laser therapy can help minimize inflammation, alter blood flow, and assist in tissue healing as well as help resolve some of the compensatory issues that develop when a patient is not loading a joint properly. We can also use therapeutic ultrasound to warm tissues or to facilitate stretching and help with extensibility and distensibility of some of those soft tissues to reorient collagen fibrils as well as help with periarticular fibrosis.
The underwater treadmill is great because higher water levels take the load of stress off the joint. If we take the water level up to the level of the greater trochanter in a 100-lb dog, for example, that dog is going to feel as if he weighs 38 lb. So, he can walk at a normal pace, starting out for about 7 to 10 minutes, and all that stress is off the joint but the dog still has to actively contract the muscles.
Once the pain is under control, we can start to lower the water level to make the exercise more challenging. This will help build muscle as well as help with maintaining range of joint motion and continuing to improve cardiovascular health and endurance.
How similar is rehabilitation in human and veterinary medicine?
Much of what we know in veterinary rehabilitation has been derived from human rehabilitation. When people go for physical therapy, they do exercises at the facility and are then given “homework” to build on what they’ve started. That way, when they come back to the facility they can continue to advance.
We do the same thing in veterinary medicine. We’ll have formal rehabilitation sessions once or twice a week with a skilled therapist, and we’ll also assign a home exercise plan. I tell owners there are 2 parts to the rehab plan: the part where you come in and your pet undergoes formal sessions, and then every day you’ll have homework so that when your dog comes back we’ll be able to advance our rehabilitation plan.
The nuts and bolts of physical rehabilitation is the home exercise plan, and core to that plan is walking, walking, walking. Once the pet gets further along in terms of improvement and comfort we can start to add in uneven terrain, inclines and declines, and stairs, depending on what we’re trying to achieve.
Regenerative Medicine
Can you talk a bit about regenerative medicine in OA? What is it exactly?
Regenerative medicine is a broad interdisciplinary field that includes any type of biologic that is focused on the repair, replacement, and/or regeneration of tissues. The overall goal is reduced pain and inflammation and improved healing of injured tissues. Regenerative medicine in OA commonly includes PRP or the combination of stem cells and PRP.
There’s a lot we know about regenerative medicine and there is even more we don’t know. The biggest misconception is that people think we are generating new tissue or growing new cartilage, and that is definitely not the case. We’re not taking a 12-year-old dog with end-stage elbow OA and injecting stem cells or PRP and all of a sudden growing new cartilage. What we are doing is taking a very high concentration of growth factors and anti-inflammatories to an area of relatively poor tissue healing with the hope that we can achieve a reduction in the inflammatory response.
Where do stem cells and PRP come from?
For PRP, we gather a blood sample that is processed through a machine that renders a solution with a higher concentration of platelets and eliminates red blood cells and certain white blood cells. Within the platelets are alpha granules that contain a rich source of growth factors and anti-inflammatory mediators. Think about when you cut yourself. A clot forms at the wound and within that clot the platelets contain these alpha granules that release various growth factors as well as cytokines. These cytokines are able to recruit reparative cells to the area of injured tissue. The clot also provides a scaffolding to which cells attach to facilitate repair. We are using PRP in a similar function.
Stem cells are typically harvested from the patient’s own fat or bone marrow. The tissue can either be sent to a lab for the stem cells to be isolated and cultured, or the tissue can be processed in-house. It should be noted that stem cells that are isolated should have unique characteristics that should be identified and characterized by the lab processing the cells; this will create a homogenous population of stem cells. Tissue that is processed in-house creates what is called either the stromal vascular fraction (SVF) for fat or bone marrow aspirate concentrate (BMAC) that is a heterogeneous population of cells with the thought that some portion of the SVF/BMAC contains stem cells but the actual amount of stem cells is unknown. Stem cells primarly provide trophic support in helping diminish tissue injury, promote neovascularization, inhibit fibrosis, and help recruit resident cells in the region for tissue repair. When stem cells are used with PRP, the PRP creates a scaffolding for the cells to attach to, which in theory may have a more beneficial effect than using either alone.
What type of research has been done with regenerative medicine?
When any new concept is introduced to patients, whether humans or animals, our first mandate is to do no harm. When used appropriately, both PRP and stem cells have been shown to be safe with minimal to no adverse effects. In addition to safety, we also need to have faith in the systems used for processing to ensure that we are delivering to our patients what we think we are. To achieve this, the systems need to be validated. However, we should use caution when using the word “validated” because there are so many factors between and within patients that can alter platelet and stem cell function, number, and collection. In addition, different collection and processing methods can have an effect on what is produced. Current work has been completed with PRP to show that the machines used for processing can provide repeatable results.2,3 To date, there is no published information on in-house processing of SVF/BMAC. Again, between- and within-patient variables will make this challenging if not impossible to standardize.
Once the systems are noted to be repeatable, then we need to determine what we want in a product and what dose and how often it needs to be given, and we need to prove efficacy through multicentered blinded placebo-controlled studies with objective outcome measures and appropriate statistical power to detect differences.
What’s interesting is that many of the translational studies using regenerative medicine for human application come from animal models, often using dogs.4 The challenge is that many of these studies are published in human journals; they’re not going to show up in our veterinary literature, so we won’t necessarily know about them. Nevertheless, extreme caution should be used when evaluating these studies as controlled tissue injuries don’t always match spontaneous injuries that are seen clinically. Also, although stem cells among species are similar there are some key differences. This highlights the need for caution that definitive conclusions about canine stem cell differentiation based on literature from other species is not made regardless of the tissue source.
What is your advice to veterinarians about regenerative medicine?
Pet owners are asking about some of these minimally invasive, nonpharmacologic approaches to OA management, and we need to be prepared to give them appropriate information and realistic expectations. Some people are jumping in headfirst, but we’re really just getting our toes wet with regenerative therapies in veterinary medicine and there are a number of things we need to evaluate to determine how to use these therapies appropriately. With OA, for example, depending on the level of changes present, the patient may require a certain type of PRP or stem cell therapy. Should every product be used in the same way, or do we take more of a patient-centered approach? How many injections do we give, and how frequently? When do we use PRP or stem cells alone, and when do we combine them? There is a lot of work yet to be done to determine how we can best use regenerative therapies to improve patient care, but I think it’s a promising technology that’s showing some benefits when used in the appropriate manner.
Other New Therapies
What other types of treatment are on the horizon?
I think in the future there will be a move toward more molecular-driven therapies rather than giving a medication to block an entire pathway. We have seen the beginnings of this in veterinary medicine with the development of a monoclonal antibody therapy directed toward nerve growth factor. In people, nerve growth factor has been shown to be a significant source of pain and inflammation associated with OA. Results of clinical trials have shown relief of OA pain for about 4 weeks in dogs and 7 days in cats. This was originally developed by a company called Nexvet Biopharma, which was acquired by Zoetis. Since the acquisition by Zoetis we have not heard any more about this promising technology.
I’m also working on a clinical trial for the use of a targeted pulsed-electromagnetic field (PEMF) therapy for OA management.
What is that?
Targeted PEMF therapy, which has been FDA approved for use in people, delivers a targeted pulse of electric current to tissue. Initially, many companies thought that a powerful magnet was needed or that “more is better,” which we now know is not the case. We’ve known since the 1970s that low-powered PEMF can help with bone healing as well as reducing inflammation. While the exact mechanisms of action are unknown, the major thought is the binding of calcium and calmodulin by the PEMF, which naturally initiates an anti-inflammatory cascade. This is accomplished by leading to the production of nitric oxide, which is a principal anti-inflammatory molecule that assists in reducing pain, improving blood flow, and reducing edema. This was a blinded placebo-controlled pilot study using objective outcome measures. We are still awaiting the initial results to determine whether a difference was noted.
References:
- Budsberg SC, Torres BT, Kleine SA, Sandberg SA, Berjeski AK. Lack of effectiveness of tramadol hydrochloride for treatment of pain and joint dysfunction in dogs with chronic osteoarthritis. J Am Vet Med Assoc. 2018;252(4):427-432. doi: 10.2460/javma.252.4.427.
- Carr BJ, Canapp SO Jr, Mason DR, Cox C, Hess T. Canine platelet-rich plasma systems: a prospective analysis. Front Vet Sci. 2016;2:73. doi: 10.3389/fvets.2015.00073.
- Franklin SP, Garner BC, Cook JL. Characteristics of canine platelet-rich plasma prepared with five commercially available systems. Am J Vet Res. 2015;76(9):822-827. doi: 10.2460/ajvr.76.9.822.
- Bozynski CC, Stanard JP, Smith P, et al. Acute management of anterior cruciate ligament injuries using novel canine models. J Knee Surg. 2016;29(7):594-603. doi: 10.1055/s-0035-1570115.
